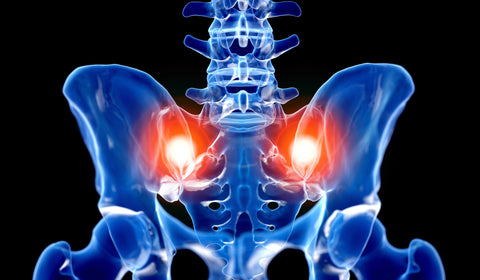
Lower back pain is one of the most common pain complaints among adults. It is estimated that 10-25% of low back pain complaints are due to SI joint dysfunction. It’s not easy to diagnose as the symptoms are vague and may also mimic the symptoms of other back conditions such as sciatica or herniated discs.
Signs that sacroiliac dysfunction is causing your back pain include:
- Dull aching on the sides of the lower back or upper buttocks
- Lower back pain that radiates into your hip or hamstrings
- Pain that is worse when you stand or walk
SI joint dysfunction can lead to pain during normal daily movements such as sitting for long periods of time, standing, walking, bending over to pick up objects, or climbing stairs. This also makes it difficult to keep up with an exercise routine, as many different movements seem to cause pain.

What is the SI Joint, and What Leads to Dysfunction
The sacroiliac joint is the junction where the pelvis meets the spine. The left and right ilium bones make up the pelvis. The 5 fused bones of the vertebrae at the bottom of the spine are the sacrum. The sacrum is connected to each ilium by strong ligaments, and this connection is what we call the SI joint. Unlike most of the joints in the body, the SI joint is meant more for stability than mobility.
The SI joint is dysfunctional if there is either too much movement in the joint or not enough. If the integrity of the supporting ligaments is compromised or if the supporting muscles do not create stability, the SI joint will move much more than is necessary. If there is excessive inflammation in the joint or sacroiliitis, movement may be decreased, leading to compression.
The SI joint mediates forces between the lower body and the upper body. In movement, the rotational force generated in the lower body is transferred up to the upper body via this joint. Functional movement is a symphony of coordinated rotations and counterrotations, flexions, and extensions happening symmetrically throughout the body. Rotation of the ribcage, the femurs, and the pelvis all play a role in pain-free movement.
When the body functions well, load and impact will be transferred efficiently, both up and down the kinetic chain. When one or more muscles do not fire to create the necessary movement or stability in a joint, another joint tends to compensate. This tends to be the root problem with SI joint dysfunction. When certain muscles are not firing in coordination with others, the SI joint can bear the brunt of the impact forces taken on by walking.
Common causes of SI joint dysfunction include
- Chronic stretching
- Muscle imbalances
- Postural asymmetries
- Scoliosis
- Laxity of the SI ligaments (as in pregnancy)
- Trauma (such as a traffic collision)
- Impact injuries (such as falling onto the buttocks)
- Sacrum or lumbar spinal fusions
- Arthritis
- Leg length discrepancy
- Heavy lifting
Common Interventions for SI Pain
Muscle Relaxers
Muscle relaxers can temporarily relieve SI joint pain by relaxing the muscles around the joint. However, this is not a long-term solution as it does not address the underlying issue causing the pain. It is recommended instead to address the root cause of the pain. We will discuss how to address the root later in this article.
Back Braces for SI Joint Pain
The idea behind back braces for SI joint pain is to create stability in the joint by providing support. The effectiveness of these braces is not widely studied and may only be beneficial for some types of SI joint pain. (Zaman, F., et al. "Non-surgical treatments for sacroiliac joint dysfunction: a systematic review." European Spine Journal 26.3 (2017): 711-720) For some people, the SI joint is already compressed and would not benefit from more pressure.
Again, the problem with back braces is you’re putting a bandaid on a deeper issue instead of addressing the root cause.
Stretching for SI Joint Dysfunction

It’s common to believe that stretching will be beneficial for SI joint pain; however, this is misinformed. While hundreds of articles titled “stretching for SI joint pain” litter the web, this is likely another band-aid approach. If stretching had any long-term benefit for SI joint dysfunction, this wouldn’t be a widespread problem. The bottom line is that stretching or yoga might provide short-term relief from the symptoms of SI joint dysfunction, but the pain will recur because the root of the issue is instability. Stretching creates more instability in a joint, not less.
Strength Training for SI Joint Dysfunction

On the surface, it seems to make sense that training the glutes and the core muscles would build some stability on which the pelvis could operate more safely. In practice, this does not seem to be the case. As discussed above, some common causes of SI joint dysfunction are muscular imbalance, postural distortion, and compression. Traditional weightlifting routines will only exacerbate these issues, not address them.
For example, traditional weightlifting would suggest performing squats for your SI joint pain because, in theory, this would strengthen the glutes. Unfortunately, this exercise puts more compression on the lumbar and sacrum region while simultaneously engraining in postural distortions and rotational imbalances. This seems to be a high-risk, low-reward scenario. Training the glutes in an arbitrary fashion without regard for how the glutes work in the gait cycle will only lead to further imbalance and SI joint pain.
SI Joint Fusion Surgery
The surgical approach to SI joint dysfunction involves fusing the sacrum and the ilium bones to stabilize the joint. While this sounds like it may be a viable option for people lacking stability through the joint, there is limited long-term data on the outcomes of this procedure. Some studies suggest that up to 46% of patients will continue to have pain after their SI joint fusion surgery. (Patel VV, Manchikanti L, Singh V, et al. Clinical outcomes of minimally invasive SI joint fusion at 2-year follow-up: a prospective study. J Pain Res. 2020;13:2079-2089. doi:10.2147/JPR.S257134 and Rudolf L, Capobianco R. Five-Year Clinical and Radiographic Outcomes After Minimally Invasive Sacroiliac Joint Fusion Using the iFuse Implant System. J Bone Joint Surg Am. 2018;100(5):400-406. doi:10.2106/JBJS.16.00770)
Like any major surgery, this procedure comes with risks such as infection, nerve injury, hardware failure, and continued or worsening pain.
Addressing SI Joint Pain Without Surgery
As mentioned previously, the SI joint tends to become dysfunctional as a result of muscular or postural imbalance, often coupled with overuse. An exercise strategy for SI joint pain should be focused on providing stability through the region by targeting the correct muscle chains.
Which muscles are involved in SI joint stability? Let’s look at the most influential muscle chain that crosses this joint.

You can see clearly in the image above that the posterior oblique sling (POS) includes the latissimus dorsi, thoracolumbar fascia, and gluteus maximus. When latissimus and gluteal muscles are activated, they create a diagonal tension through the thoracolumbar fascia, which helps to prevent excessive movement of the SI joint during activities like walking and running. In fact, this is one of the primary muscle chains that create the movement of walking. When the POS is properly strengthened, you’ll have more ease of movement in daily activities and more intrinsic stabilization and decompression of the spine and hips.
According to studies, the POS may be an important factor in preventing SI joint dysfunction and improving outcomes in individuals with SI joint pain. One study published in the Journal of Orthopaedic and Sports Physical Therapy found that a strengthening program targeting the posterior oblique sling system was effective in reducing pain and improving function in individuals with SI joint pain. (Selkowitz, D. M., Beneck, G. J., & Powers, C. M. (2016). A Specific Exercise Program and Modification of Postural Alignment for Treatment of SI Joint Dysfunction in Female Runners: A Randomized Controlled Trial. Journal of Orthopaedic & Sports Physical Therapy, 46(7), 581-591. doi: 10.2519/jospt.2016.6280)
A review article published in the Journal of Anatomy in 2014 found that the posterior oblique sling system plays a crucial role in controlling the shear and compressive forces that occur at the SI joint during normal activities. The researchers concluded that disruption of this sling system might contribute to SI joint dysfunction. (Vleeming, A., Schuenke, M. D., Masi, A. T., Carreiro, J. E., Danneels, L., & Willard, F. H. (2014). The posterior oblique sling and its contribution to pelvic stability, low back pain, and trunk rotation: a review. The Journal of Anatomy, 224(4), 363-376.)
You might wonder which exercises are good for targeting the posterior oblique slings. Because the oblique slings are the primary drivers in walking and running, it makes sense that using gait-based movements such as the Functional Patterns Contralateral Step Pull would facilitate this connection. This pattern is a rotational movement that coordinates opposite limbs.
Gait-based training has many benefits that carry over into life:
- Muscle development through the sling system
- Coordination of opposite limbs
- Increased spatial awareness
- Builds efficient walking and running
- Posture improvement and spinal decompression
Conclusion

In closing, the causes of SI joint pain need to be addressed in order to stabilize the joint properly. After examining the traditional treatments for SI joint dysfunction, it seems they are primarily isolated band-aid approaches and not long-term solutions for the root causes of SI joint pain. Dysfunction of the SI joint does not occur in isolation. Any approach that will provide long-term relief for SI joint pain will strive to build functional symmetry of muscle development and movement capability.
If you’re suffering from SI joint issues, you should begin your journey by examining where your asymmetries are. How well do you rotate to the left vs. the right? Are your glutes functioning symmetrically? Do your lats work in conjunction with your glutes?
If this sounds overwhelming, like you would have no idea where to start, the Functional Patterns 10-week course covers these basic concepts. This course takes you through the progressive steps of in-depth myofascial release, developing solid core tension, and building the connections between the upper and lower body. Building stability through the hips and core is the foundation of Functional Patterns training. Utilizing this progressive system will enable anyone with SI joint pain to find relief by solving the root causes of the problem.
The bottom line is that SI joint pain is a solvable problem when you address the body’s fundamental movement patterns. With Functional Patterns, you can resolve your SI joint pain while simultaneously improving your economy of motion and developing functional muscle. Take the first step to correcting your posture and movement issues: start with the 10-week online course today.







